Basic Pathological Processes
Abnormal patterns detected during needle examination
Spontaneous Activity
Fibrillations and Positive Waves
When muscle fibers lose nerve supply, acetylcholine receptors redistribute across the fiber surface rather than concentrating at the end-plate. This causes spontaneous depolarization when acetylcholine molecules reach the fiber, generating detectable action potentials.
Positive Sharp Wave
Describes a very sharp positive deflection off the baseline followed by a slower return with occasional negative phases. These waves reach up to 1 mV amplitude and persist up to 50 milliseconds, discharging rhythmically with abrupt starts and stops.

Fibrillation Potential
Short-duration (less than 3 msec) and low-amplitude (less than 300 µV) potentials occurring in semi-rhythmic runs (less than 30/second). They emerge two to three weeks post-injury, develop earlier in proximal muscles, and may persist decades after denervation, though frequency diminishes over time.

Fasciculations
Spontaneous discharge of entire motor units in random patterns. Benign fasciculations appear monophasic or diphasic at 0.8-second intervals in normal individuals experiencing fatigue. Malignant fasciculations, associated with motor neuron disease, display longer intervals (~3.5 seconds) and complex morphology.
Complex Repetitive Discharges
Long trains of rapidly-firing potentials (20-40/sec or higher) with abrupt onset/termination. These maintain constant size and frequency throughout discharge. Commonly observed in polymyositis, Duchenne muscular dystrophy, and various neuropathic conditions.

Myokimic Discharges
Spontaneous bursts of rapidly-firing potentials recurring at regular 2-10 per second intervals, unaffected by voluntary effort, accompanying clinical myokymia.
Neuromyotonia
Very high-frequency discharges in long trains/bursts with characteristically decreasing amplitude, creating myotonic-like sounds. Typical of Isaac’s syndrome.
Myotonia
The distinctive “dive bomber” sound results from high-frequency discharges varying in amplitude and frequency, ranging 150-20/second. Triggered mechanically, electrically, or by needle insertion. Cold temperatures enhance rather than reduce myotonic discharges.
Voluntary Activity
The Neurogenic Motor Unit
Complete Transection Scenario:
After nerve repair, regenerating axons reach muscle fibers at scattered intervals, forming small (100-200 µV), short-duration (3-5 ms), polyphasic “nascent” potentials appearing in the first two months. Within four to eight months, these units normalize in amplitude and duration.
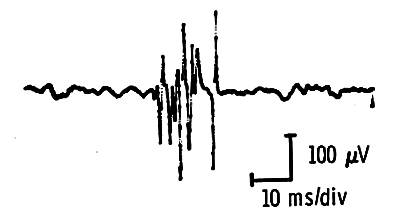
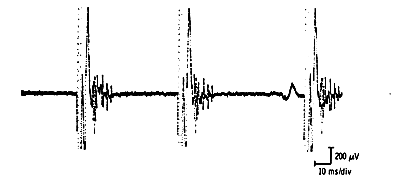
Partial Nerve Injury (More Common):
Collateral sprouting allows denervated fibers to seek innervation from adjacent axons. This reinnervation increases motor unit size while introducing asynchrony between original and newly-acquired fibers. Long-duration, polyphasic motor units with unstable components indicate active reinnervation.
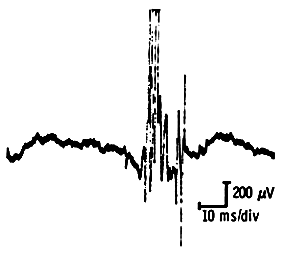
Within six to eight weeks, newly-incorporated fibers synchronize with surviving units. The resulting chronic neurogenic motor unit features high amplitude, long duration, and characteristic “thundery noise.” Units exceeding 10 mV constitute “giant potentials.”
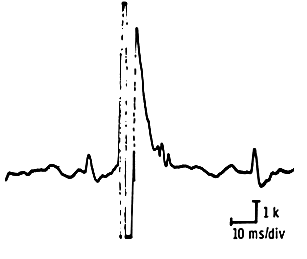
The Myopathic Lesion
When muscle fibers degenerate while nerves remain largely intact, typical early changes include reduced motor unit duration and amplitude. Motor units display high phase numbers and erratic desynchronization. Characterized by “scratchy metallic sound” comparable to hail on tin. These units recruit in large numbers at minimal voluntary effort, producing full interference patterns with moderate contraction.
Neuromuscular Transmission Defects
Severely impaired transmission excludes muscle fibers from motor units moment-to-moment, creating visible shape variations in motor unit potentials. Affected muscles show decrement on repetitive stimulation studies.