Needle Examination Work-Ups
Structured protocols for needle testing
The needle examination requires broad-range work-ups for general pathological process groups. Clinical understanding of spinal segments for upper and lower extremity muscles is essential for proper interpretation.
These work-ups enable:
- Unbiased patient assessment, allowing discovery of diagnoses beyond initial referral suspicions
- Simplified approaches to disease groups adaptable to specific conditions
Five general work-ups are described, similar to nerve conduction study approaches: routine upper extremity, routine lower extremity, peripheral neuropathy, anterior horn cell disease, and myopathy.
Routine Upper Extremity
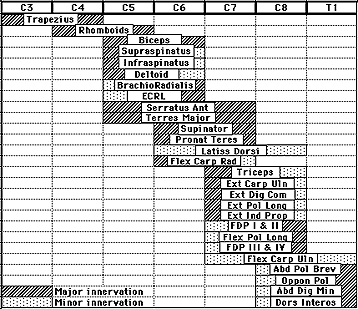
This work-up addresses roots, plexus, entrapment, and traumatic neuropathies affecting the upper extremity. It emphasizes sampling muscles from different upper extremity nerves at C5-T1 root levels.
Sampled muscles include:
- First dorsal interosseous (ulnar C8, T1)
- Flexor pollicis longus (anterior interosseous C7,8)
- Flexor carpi radialis (median C7)
- Brachioradialis (radial C5,6)
- Triceps (radial C7,8)
- Deltoid (axillary C5,6)
Root lesion assessments should include appropriate paraspinal levels.
Routine Lower Extremity
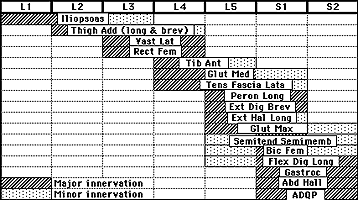
Designed for roots, plexus, entrapment, and traumatic neuropathies of the lower extremity, this work-up emphasizes muscles from different lower extremity nerves at L3-S2 root levels.
Sampled muscles include:
- Extensor digitorum brevis or extensor hallucis longus (peroneal L5-S1)
- Flexor digitorum longus (posterior tibial L5-S1,2)
- Tibialis anterior (peroneal L4,5)
- Medial gastrocnemius (posterior tibial S1,2)
- Vastus lateralis (femoral L3,4)
- Gluteus medius (superior gluteal L4,5 and S1)
Root lesion work-ups should sample appropriate paraspinal levels.
Peripheral Neuropathy
This work-up emphasizes distal muscle sampling, as these are typically more involved in neuropathic processes.
Components include:
- Routine upper extremity examination plus abductor digiti minimi
- Routine lower extremity examination plus abductor hallucis
Anterior Horn Cell
The primary objective involves sampling muscles across widespread root distribution to exclude multiple motor radiculopathies.
Requirements include:
- Minimum of two routine extremity work-ups
- Routine upper extremity study
- Routine lower extremity study
- Additional upper or lower extremity based on clinical involvement areas
- Tongue examination
Myopathy
This work-up addresses various myopathy groups, myotonias, and Lambert-Eaton syndrome, with emphasis on proximal muscles.
Components include:
- Modified routine upper extremity (deleted flexor pollicis longus; added biceps and infraspinatus)
- Modified routine lower extremity (deleted flexor digitorum longus; added thigh abductors and iliacus)
- Paraspinal muscle sampling in inflammatory myopathies to enhance diagnostic yield
Neuromuscular Transmission
Single fiber EMG has transformed traditional neuromuscular transmission defect work-ups. While moment-to-moment motor unit potential variations are useful, jitter analysis by single fiber EMG is a much more sensitive means to study defects in transmission.
This specialized technique uses a 25 µm needle electrode tip with side port recording, positioning near two muscle fibers from the same motor unit. Synchronously firing potentials allow measurement of interpotential interval variation across multiple tracings, calculating mean interpotential interval and standard deviation.
In neuromuscular transmission disorders, jitter increases early in illness progression, before repetitive stimulation tests become positive. Later stages show impulse blocking from total neuromuscular transmission failure, causing potential disappearance on screen.