Nerve Conduction Work-Ups
Systematic testing protocols and approaches
This page outlines standardized protocols for conducting nerve conduction studies based on clinical presentation. These guidelines must be general enough to include most of the abnormalities seen in this group while remaining flexible enough to allow adjustments as needed.
Five Standard Work-Up Protocols
Routine Upper Extremity
Designed for evaluating root/plexus lesions and compression or traumatic injuries in the upper arm. The protocol includes median and ulnar nerve sensory and motor studies with F-waves, plus radial sensory testing.
Routine Lower Extremity
For assessing lower limb root or plexus damage. This involves sural and superficial peroneal sensory studies, peroneal and posterior tibial motor studies with F-waves, and H-reflex evaluation when indicated.
Generalized Neuropathic Process
Combines both upper and lower extremity routines with H-reflex studies for systemic neuropathies and anterior horn cell disorders.
Myopathy
Uses limited testing (median and sural sensory; peroneal motor) since muscle diseases typically show minimal nerve conduction abnormalities.
Neuromuscular Junction
Divided into presynaptic and postsynaptic variants. Presynaptic disorders (Lambert-Eaton) show post-exercise amplitude facilitation. Postsynaptic testing (myasthenia gravis) uses repetitive stimulation at 2 Hz to detect decrements exceeding 10 percent.
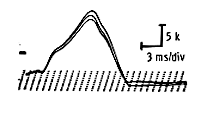
A decrease in the amplitude or area of more than 10 percent between the first and fourth potential is interpreted as a positive decrement.
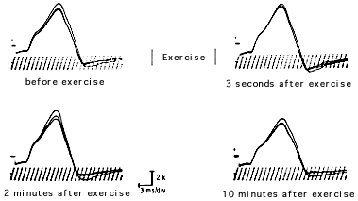
Typically a myasthenic response will show a pre-exercise decrement between the first and fourth response exceeding 10 percent. This decrement is partially and at times totally corrected immediately after exercise.